Giuseppe Faraco, MD, Ph.D.
Assistant Professor of Neuroscience
Finbar and Marianne Kenny Research Scholar in Neurology
Overview
The brain is a major target of the end-organ damage produced by hypertension and other vascular risk factors including excessive salt consumption. Vascular risk factors have long been associated with cerebrovascular diseases and cognitive impairment. Both hypertension and a diet rich in salt have been linked to the cerebral small vessel disease underlying vascular cognitive impairment, a condition associated with endothelial dysfunction and reduced cerebral blood (CBF). Despite the benefits of anti-hypertensive therapy, the burden of disease caused by hypertension remains substantial, especially in the brain. In addition, strategies aimed at reducing salt intake have been largely unsuccessful and salt consumption across the world is still higher than what recommended by the American Heart Association or the World Health organization.
Cerebral blood vessels are uniquely susceptible to the deleterious effects of salt and hypertension. We have shown that both hypertension and high salt intake disrupt neurovascular control mechanisms that assure an adequate cerebral blood supply. Loss of these vital homeostatic responses compromises the blood supply to the brain and increases the susceptibility of the brain to vascular insufficiency and ischemic damage. The elucidation of the molecular mechanisms underlying such harmful effects is a necessary step for developing new approaches to prevent stroke and dementia.
Our research is particularly focused in elucidating the specific cellular targets through which hypertension and other vascular risk factors alters neurovascular function, and their eventual link to cognitive impairment. Over the last years, we have shown that perivascular macrophages, innate immune cells that closely associate with cerebral arterioles, are critical for mediating oxidative stress, impairing arteriolar function in hypertension and inducing cognitive impairment. Remarkably, depletion of perivascular macrophages was able not only to improve vascular function of hypertensive mice but it also rescued the cognitive impairment induced by hypertension, suggesting that these cells might play a key role in mediating the detrimental effects of hypertension on cognition. Furthermore, we recently showed that a diet rich in sodium has deleterious effects on the cerebral endothelium which play an essential role in regulating CBF by releasing important dilator and constrictor molecules. These effects are dependent on expansion of IL-17-producing T-helper lymphocytes (TH17 cells) in the small intestine, resulting in a marked increase in the cytokine IL-17 which acts on cerebral endothelial cells reducing their ability to produce nitric oxide, a crucial regulator of cerebral blood flow. We also demonstrated that the endothelial dysfunction induced by high sodium intake is associated with cognitive impairment. Remarkably, in a follow-up study, we have shown that dietary salt induces accumulation of hyperphosphorylated tau, a microtubule associated protein and a hallmark of Alzheimer’s pathology, followed by cognitive dysfunction, effects prevented by restoring nitric oxide production in cerebral endothelial cells.
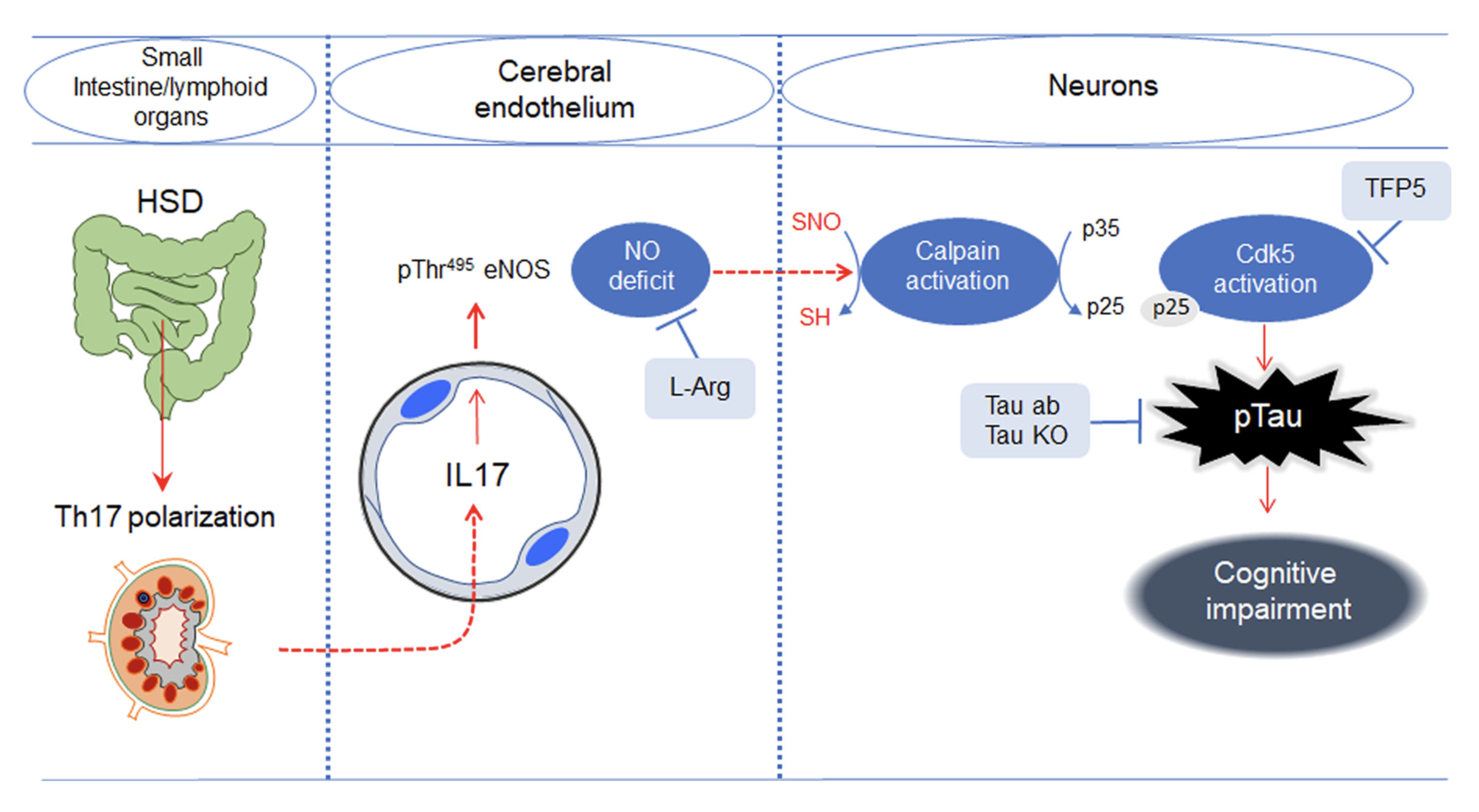
Cartoon depicting the mechanisms by which high salt diet leads to tau phosphorylation and cognitive impairment (Nature. 574:686, 2019).
Achievements
- Grant from NINDS, 1R01NS130045-01 (2022-2027) “Gut Immunity, Neurovascular dysregulation and Cognitive Impairment”
- Grant from Cure Alzheimer’s Fund (2021-2023) “Gut microbiota, endothelial dysfunction and tau-mediated cognitive impairment”
- Grant from Cure Alzheimer’s Fund (2018-2020) “Dietary salt, tau phosphorylation and cognitive impairment”
- Scientist Development Grant Award from the American Heart Association (2015-2018) "Role of immune cells in Angiotensin II-mediated neurovascular dysfunction”
Selected Publications
Faraco G, Hochrainer K, Segarra SG, Schaeffer S, Santisteban MM, Menon A, Jiang H, Holtzman DM, Anrather J, Iadecola C. Dietary salt promotes cognitive impairment through tau phosphorylation. Nature. 574:686, 2019
Faraco G, Brea D, Garcia-Bonilla L, Wang G, Racchumi G, Chang H, Buendia I, Santisteban MM, Segarra SG, Koizumi K, Sugiyama Y, Murphy M, Voss H, Anrather J, Iadecola C. Dietary salt promotes neurovascular and cognitive dysfunction through a gut-initiated TH17 response. Nat Neurosci. 21:240, 2018
Faraco G, Park L, Anrather J, Iadecola C. Brain perivascular macrophages: characterization and functional roles in health and disease. J Mol Med (Berl). 95:1143, 2017
Faraco G, Sugiyama Y, Lane D, Garcia-Bonilla L, Chang H, Santisteban MM, Racchumi G, Murphy M, Van Rooijen N, Anrather J, Iadecola C.Perivascular macrophages mediate the neurovascular and cognitive dysfunction associated with hypertension. J Clin Invest. 126:4674, 2016.
Garcia-Bonilla L, Faraco G, Moore J, Murphy M, Racchumi G, Srinivasan J, Brea D, Iadecola C, Anrather J. Spatio-temporal profile, phenotypic diversity, and fate of recruited monocytes into the post-ischemic brain. J Neuroinflammation. 13:285, 2016.
Benakis C, Brea D, Caballero S, Faraco G, Moore J, Murphy M, Sita G, Racchumi G, Ling L, Pamer EG, Iadecola C, Anrather J. Commensal microbiota affects ischemic stroke outcome by regulating intestinal γδ T cells. Nat Med. 22:516, 2016.
Faraco G, Park L, Zhou P, Lou W, Paul SM, Anrather J, Iadecola C. Hypertension enhances Aβ-induced neurovascular dysfunction, promotes β-secretase activity and leads to amyloidogenic processing of APP. J Cereb Blood Flow Metab. 36:241, 2016.
Faraco G, Iadecola C. Hypertension: A Harbinger of Stroke and Dementia. Hypertension. 62:810, 2013
Faraco G, Moraga A, Moore J, Anrather J, Pickel VM, Iadecola C. Circulating Endothelin-1 Alters Critical Mechanisms Regulating Cerebral Microcirculation. Hypertension. 62:759, 2013.
Capone C, Faraco G, Peterson JR, Coleman C, AnratherJ, Milner TA, Pickel VM, Davisson RL, and Iadecola C: Central Cardiovascular Circuits Contribute to the Neurovascular Dysfunction in Angiotensin II Hypertension. The Journal of Neuroscience 32:4878, 2012.

